I’ve hunted high and low for something that worked for my own stubborn foot blisters. What I found in 2009 was ENGO Blister Patches. Here’s why I love them.
Blister Prevention
Find everything you need to treat your blisters and stop them coming back, for good!
Blister Prevention Shop
Visit our store to try our own best selling products and brands I whole heartedly recommend. to both prevent and treat any foot blisters. Blister Patches, Gel Toe Protectors, Blister Kits and other products you will love.
30+ Years Clinical Experience
I’ve been helping people prevent and treat foot blisters in my podiatry clinic, on the sporting field and track-side at running events for thirty years; and online through this website and YouTube channel for fifteen years.
Courses, Articles, Videos
Thousands have used my advice to fix their blisters and hundreds have stayed in their race after I have treated their blisters. I know anyone can do this and I’m here to tell you that you don’t need to be a podiatrist to do it.
FOOT BLISTER PREVENTION & TREATMENT
Foot blisters are one of the most common foot injuries in sport and everyday life. Yet their cause is largely misunderstood. On this site, you’ll find lots of blister prevention tips on how to match the right products and techniques to treat any foot blister you currently have.





Not sure what to put on it? Get my 5-step blister treatment system to avoid the common mistakes and help it heal faster.

Let me help you take an inside-out approach to the cause of your blister so you can choose the right blister prevention for it.
MY GO-TO BLISTER PRODUCT
I’ve hunted high and low for something that worked for my own stubborn foot blisters. What I found in 2009 was ENGO Blister Patches. Here’s why I love them.
HOW TO CHOOSE YOUR PATCH
ENGO Patches come in 4 shapes. Read this article to find out how to choose the right patch for your foot blister.
BUY ENGO PATCHES
Buy your ENGO Heel Pack, ENGO 4-Pack, ENGO 6-Pack, ENGO Rectangle Pack, ENGO 30-Pack and ENGO Combo Pack from our secure online store.
We ship worldwide from US and Australia.
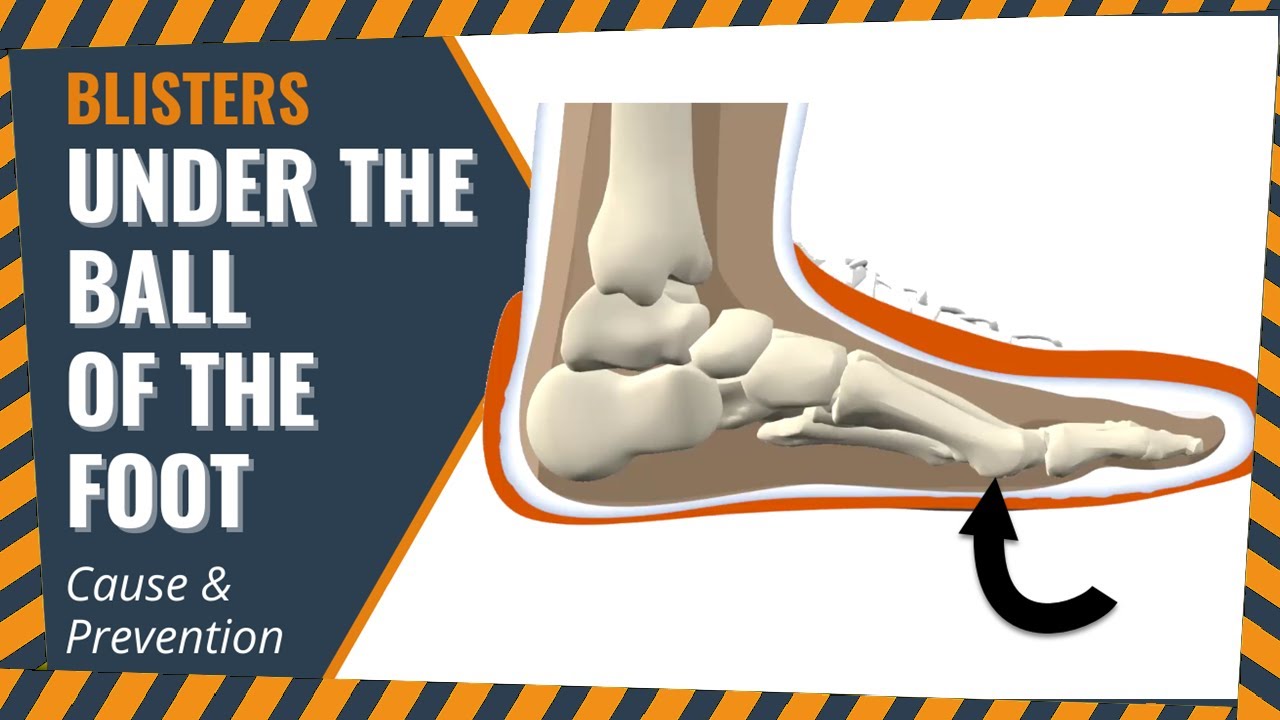
What Causes Foot Blisters?
We often blame heat, moisture and friction.
But there's more to blisters than meets the eye.
Learn more in the video below.

Our YouTube Video Resource Hub
Our online community is vibrant and we have been providing a tonne of helpful video content to people all across the world for over 8 years.
Check out some of our most viewed videos below or view our channel.
TOP 3 MISTAKES OF FOOT BLISTER TREATMENT
LET ME SHOW YOU WHAT THESE MISTAKES ARE NOW, SO YOU CAN AVOID THEM, AS OF TODAY.
Have you ever used a hydrocolloid blister dressing? You know, those yellow, gummy kind of blister dressings, like Compeed? I bet you’ve made one of these common mistakes – I see people make them all the time. In this video, I’m going to show you what these mistakes are:
So you can start using Compeed properly
So you stop making your blisters worse



COMMON PROBLEMS
On this site, you’ll find lots of tips on how to match the right products, tools and techniques to treat any foot blister you currently have (including blood blisters).
Thousands have used my advice to fix their foot blisters and have stayed in their race after I have personally treated their blisters. I’m here to tell you that you don’t need to be a podiatrist to do this.
Our Customers Love Us

HI, I’M REBECCA RUSHTON
I’VE BEEN HELPING PEOPLE PREVENT AND TREAT FOOT BLISTERS IN MY PODIATRY CLINIC, ON THE SPORTING FIELD AND TRACK-SIDE AT RUNNING EVENTS FOR THIRTY YEARS; AND ONLINE THROUGH THIS WEBSITE AND YOUTUBE CHANNEL FOR FIFTEEN YEARS.
Hundreds of thousands of people all over the world have watched my videos on treating blisters on feet, including blood blister treatment and blister popping techniques. Thousands have used my advice to fix their blisters and hundreds have stayed in their race after I have treated their blisters. I know anyone can do this and I’m here to tell you that you don’t need to be a podiatrist to do it.

SUBSCRIBE TO OUR NEWSLETTER
SUBSCRIBE TO OUR NEWSLETTER TODAY, AND YOU’LL BECOME A VIP SUBSCRIBER, WITH IMMEDIATE ACCESS TO THE VASELINE REPORT.
Benefits:
The Vaseline Report – right now
My best tips, tricks and insights
The latest blister news and products